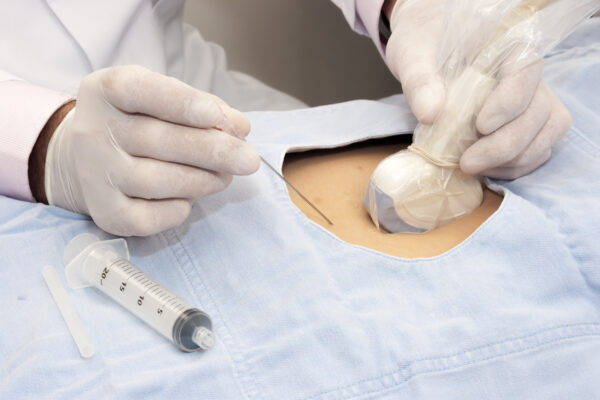
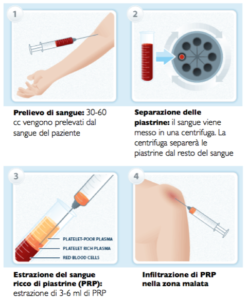
useful in patients suffering from arthritic or rheumatic joint pain who do not respond to conservative therapies (drugs and / or physiotherapy), and where it is necessary to reduce inflammation or nourish the cartilage and synovium. The infiltration, carried out under ultrasound guidance for a precise visualization of the target, consists in the injection of drugs (with anti-inflammatory and / or lubricating activity) inside the joints (hip, knee, shoulder, lumbar and cervical facets, small joints of the hand and foot), in order to reduce painful symptoms.
Hyaluronic acid:
Hyaluronic acid is a substance naturally produced by the human body that can be found in the connective tissue of the skin, in the cartilage or in the tendons of the joints.
The synovial fluid of the joint cavities confers viscosity and prevents the bones from coming into contact with each other during movement, cushioning the blows that arrive at the joint.
Hyaluronic acid contributes to the lubrication mechanisms under load conditions and tries to protect the tissue from the penetration of inflammatory cells or lytic enzymes.
When due to aging or specific pathologies, hyaluronic acid does not regenerate after being metabolized and is missing, local injections can be used.
In joints affected by severe arthrosis, the inflammatory fluid is poor in both elasticity and viscosity and therefore the purpose of the intra-articular injection of hyaluronic acid, called viscosupplementation, is to restore the viscoelastic properties of the synovial fluid.
Hyaluronic acid stimulates anabolic activity with the production of new cartilage. The action on humans is anti-inflammatory and analgesic, the better the more the pathological situation is at the beginning.
The use of intra-articular therapy with hyaluronic acid is indicated in patients who have not responded to physiotherapy and / or pharmacological treatments.




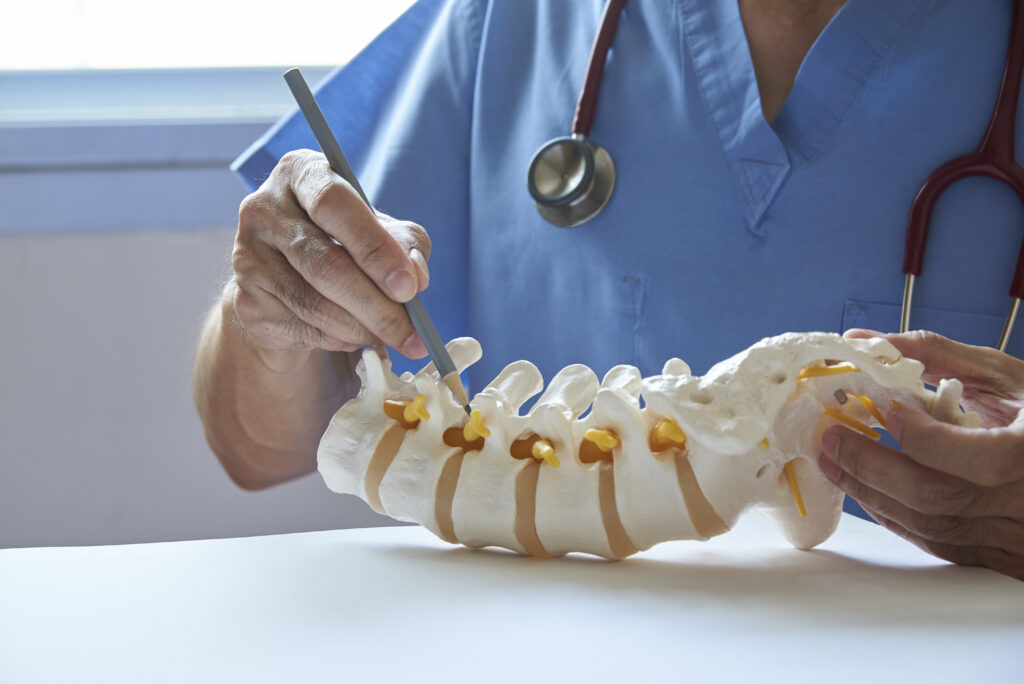


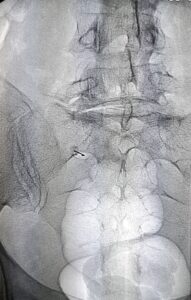 The insertion of the needle into the conjugation foramen, under fluoroscopic guidance, allows to reach the root affected by the pathological process. The target of the procedure is confirmed by the use of contrast liquid. The infiltration of the root with anti-inflammatory drugs, such as slow-release cortisone or ozone, allows the resolution of pain.
The insertion of the needle into the conjugation foramen, under fluoroscopic guidance, allows to reach the root affected by the pathological process. The target of the procedure is confirmed by the use of contrast liquid. The infiltration of the root with anti-inflammatory drugs, such as slow-release cortisone or ozone, allows the resolution of pain.
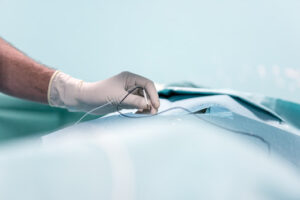 Percutaneous electrical neuromodulation is a method used for the treatment of peripheral neuropathies, occipital neuralgia and chronic post-surgical pain. Through one or more probes placed under local anesthesia just under the skin; a low voltage electric field alters the “damaged” state of the nerves, resulting in pain relief.
Percutaneous electrical neuromodulation is a method used for the treatment of peripheral neuropathies, occipital neuralgia and chronic post-surgical pain. Through one or more probes placed under local anesthesia just under the skin; a low voltage electric field alters the “damaged” state of the nerves, resulting in pain relief.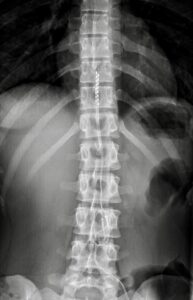

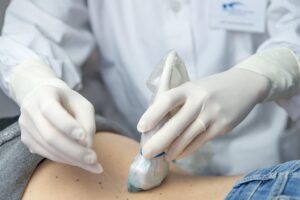 sotto guida ecografica, permette di ridurre la sintomatologia dolorosa grazie all’iniezione di farmaci con attività antinfiammatoria
sotto guida ecografica, permette di ridurre la sintomatologia dolorosa grazie all’iniezione di farmaci con attività antinfiammatoria